Presque vu (from French, meaning “almost seen”) is the sensation of being on the brink of an epiphany. Often very disorienting and distracting, presque vu rarely leads to an actual breakthrough. Frequently, one experiencing presque vu will say that they have something “on the tip of their tongue .”
In life, my focus often becomes searing, too often on folly, or distractions, but on occasions this ”fixation” is a great friend.
One fixation, was how to feed our daughter, once solids started, how to not undo all the strides Arya had made. We failed hopelessly, but Arya knew, she found Olives, she knew what they gave to her, yet her father had studied decades and failed to complete a great picture, until Arya compelled it, then gave it us when we scrambled in our minds dirt.
The smell (hexanol) compounds in Olive Oil, are hugely medicinal. The phenolic content is also medicinal, these are crucial factors, in the Liver, Pancreas, Gallbladder, Sphincter all being stimulated to secrete, contract and function (Tryptophan, Cholecystokinin, Serotonin, Insulin et al). An essay on this core bio-chemistry will follow, suffice to say, it’s important and deeply complex stuff, Arya just knew:
https://www.researchgate.net/publication/221923408_Olive_Oil_Composition_Volatile_Compounds
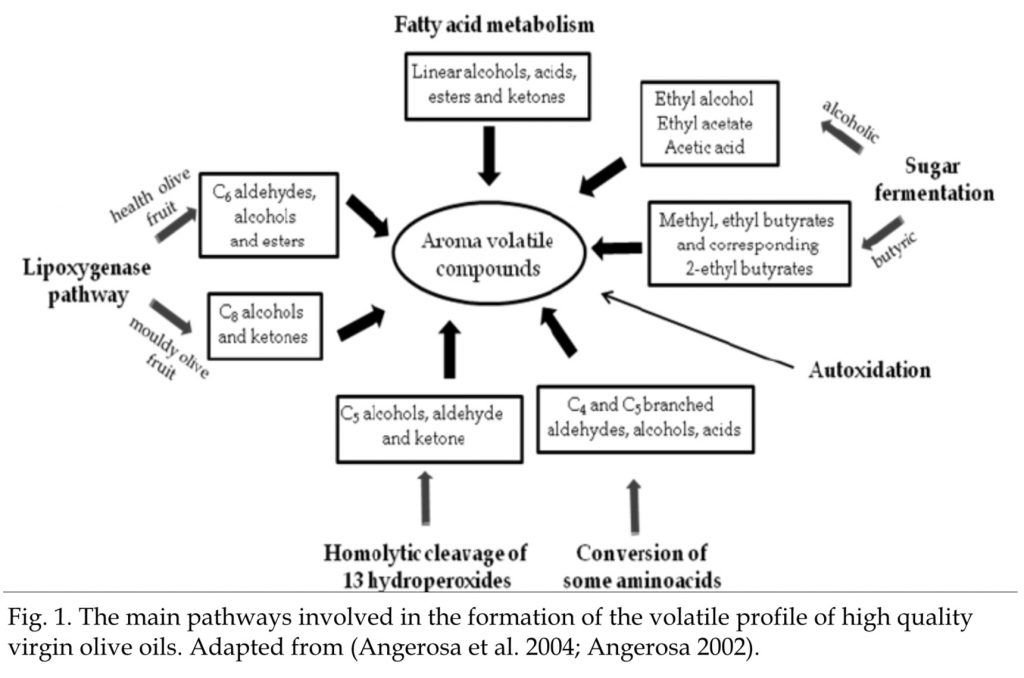
This similar theme, of Presque Vu, was found in Arya when we stimulated our friendly bacteria by making Kombucha. After months of this noble adventure, Daddy had become proficient, to the point everybody seemed to like my Kombucha, especially an Organic Apple, Carrot and Ginger second ferment blend.
When trying differing Green Teas, Sencha smooth, delicate. Others like Chun Mee more powerfully effervescent but also more acidic (Sencha for low fizz gently, Chun Mee for high fizz we had mostly settled upon), it was suggested out of the blue by Arya that using Artichoke may yield better results ”Ummm, I think it would be better if you used Artichoke Daddy”.

Daddy, being a man of considerable age and experience, nonchalantly entertained Aryas words, while my Ego dismissed this, as Arya after finding Olives, found Artichokes. So, naturally I listened and reflected that I would research, but was not sure the taste would be what we sought.
Then, to my astonishment (and, I really should have known better, by then), Arya knew this:
Malbaša et al. (2001) used the tubers of composite Jerusalem Artichoke(Helianthus tuberosus L.). They found that the drink obtained could be considered a dietary product because it had a low concentration of sugars after the fermentation process (28 °C/21 days) and the presence of inulo-oligosaccharides.
https://www.sciencedirect.com/science/article/abs/pii/S1878450X20301499
So, Arya yet again, knew or had the mind to hear, that qualities beyond my fathom, were inherent, in foods she was drawn to.
If experience hadn’t taught me otherwise, it would seem impossible.
The inulo-oligosaccharides, are very powerful sugar feeders of friendly bacteria!!! Our invisible resident, but endangered, Alchemists.
Results: Overall, nine original articles reported the effects of inulin on microbiome composition in adult humans, most of them being randomized, double-blind, placebo-controlled trials (n = 7)… The most consistent change was an increase in Bifidobacterium. Other concordant results included an increase in relative abundance of Anaerostipes, Faecalibacterium, and Lactobacillus, and a decrease in relative abundance of Bacteroides after inulin supplementation.
https://pubmed.ncbi.nlm.nih.gov/31707507/
To note, research is more and more showing, the supplementation of Inulin and/or Pectin has great benefits to out resident Alchemical potency, the younger the person, the stronger or more enduring this recolonisation effect may be (on top of cutting back on processed sugars and oxygen stifling oils).
How was it possible? After researching years, decades, that my 4year old (at that time), knew much, much, better than me?!
Thank heavens she did. Slowly we are catching her up. These days, we share a Kombucha with dinner and a spoonful of Inulin (Cake mix, the girls call it!). Though I never did make the Kombucha with it!
Blessings have been showered upon us.

Thank you Arya for bringing the knowing.











 www.sciencedirect.com
www.sciencedirect.com
