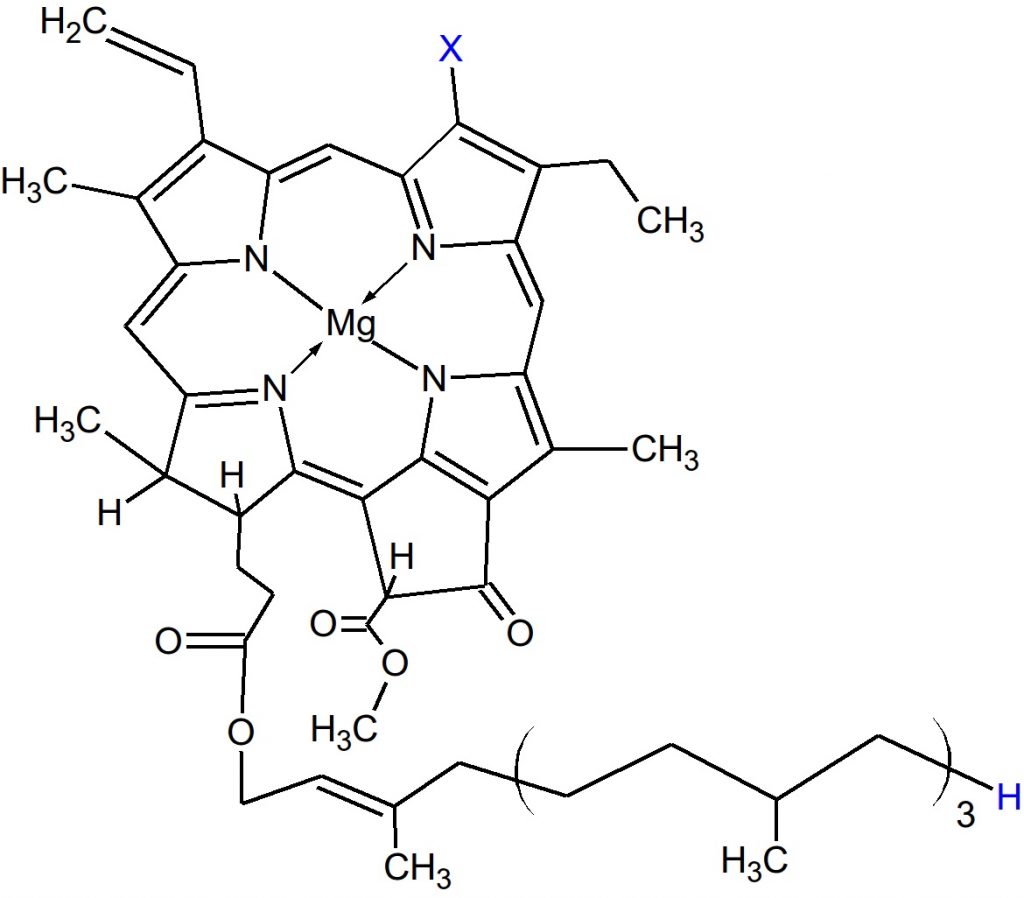
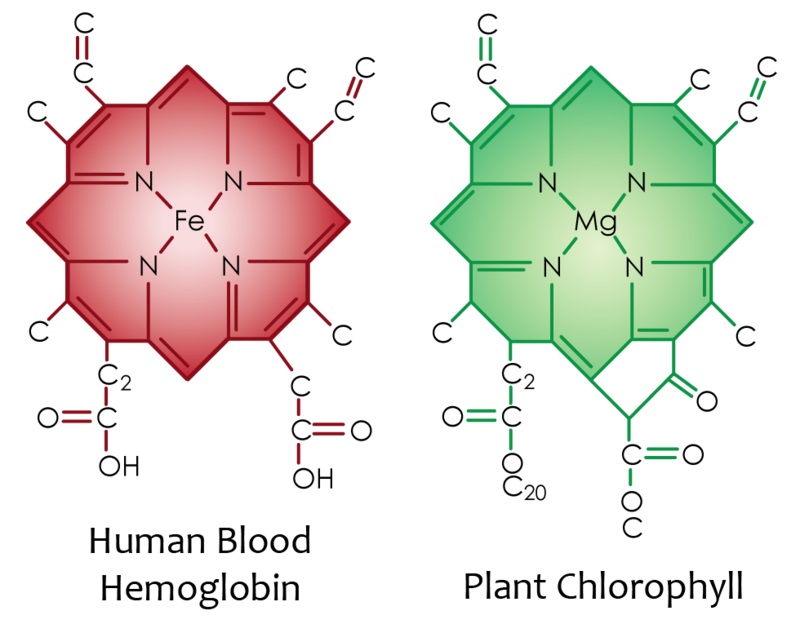
ChooseLife : Here will begin a cursory search into the scientific literature, regarding Magnesium. From the start I should note, that Reams said Chlorophyll was vital to the Liver, that for the Liver to supply the Pancreas with sufficient enzymes for it to regulate sugars properly, we need equivalent to 3oz of green juice daily (probably more nowadays), at the centre of Chlorophyll? Magnesium:
The Role of Magnesium in Neurological Disorders
Anna E. Kirkland,1Gabrielle L. Sarlo,1 and Kathleen F. Holton2,3,
Abstract
Magnesium is well known for its diverse actions within the human body. From a neurological standpoint, magnesium plays an essential role in nerve transmission and neuromuscular conduction.
It also functions in a protective role against excessive excitation that can lead to neuronal cell death (excitotoxicity), and has been implicated in multiple neurological disorders.
Due to these important functions within the nervous system, magnesium is a mineral of intense interest for the potential prevention and treatment of neurological disorders.
Current literature is reviewed for migraine, chronic pain, epilepsy, Alzheimer’s, Parkinson’s, and stroke, as well as the commonly comorbid conditions of anxiety and depression.
Previous reviews and meta-analyses are used to set the scene for magnesium research across neurological conditions, while current research is reviewed in greater detail to update the literature and demonstrate the progress (or lack thereof) in the field. There is strong data to suggest a role for magnesium in migraine and depression, and emerging data to suggest a protective effect of magnesium for chronic pain, anxiety, and stroke. More research is needed on magnesium as an adjunct treatment in epilepsy, and to further clarify its role in Alzheimer’s and Parkinson’s. Overall, the mechanistic attributes of magnesium in neurological diseases connote the macromineral as a potential target for neurological disease prevention and treatment.
Keywords: magnesium, excitotoxicity, glutamate, migraine, chronic pain, epilepsy, Alzheimer’s, Parkinson’s, stroke
Full Paper : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6024559/
Rapid recovery from major depression using magnesium treatment.
Abstract
Major depression is a mood disorder characterized by a sense of inadequacy, despondency, decreased activity, pessimism, anhedonia and sadness where these symptoms severely disrupt and adversely affect the person’s life, sometimes to such an extent that suicide is attempted or results.
Antidepressant drugs are not always effective and some have been accused of causing an increased number of suicides particularly in young people.
Magnesium deficiency is well known to produce neuropathologies. Only 16% of the magnesium found in whole wheat remains in refined flour, and magnesium has been removed from most drinking water supplies, setting a stage for human magnesium deficiency.
Magnesium ions regulate calcium ion flow in neuronal calcium channels, helping to regulate neuronal nitric oxide production. In magnesium deficiency, neuronal requirements for magnesium may not be met, causing neuronal damage which could manifest as depression.
Magnesium treatment is hypothesized to be effective in treating major depression resulting from intraneuronal magnesium deficits. These magnesium ion neuronal deficits may be induced by stress hormones, excessive dietary calcium as well as dietary deficiencies of magnesium.
Case histories are presented showing rapid recovery (less than 7 days) from major depression using 125-300 mg of magnesium (as glycinate and taurinate) with each meal and at bedtime. Magnesium was found usually effective for treatment of depression in general use. Related and accompanying mental illnesses in these case histories including traumatic brain injury, headache, suicidal ideation, anxiety, irritability, insomnia, postpartum depression, cocaine, alcohol and tobacco abuse, hypersensitivity to calcium, short-term memory loss and IQ loss were also benefited. Dietary deficiencies of magnesium, coupled with excess calcium and stress may cause many cases of other related symptoms including agitation, anxiety, irritability, confusion, asthenia, sleeplessness, headache, delirium, hallucinations and hyperexcitability, with each of these having been previously documented. The possibility that magnesium deficiency is the cause of most major depression and related mental health problems including IQ loss and addiction is enormously important to public health and is recommended for immediate further study. Fortifying refined grain and drinking water with biologically available magnesium to pre-twentieth century levels is recommended.
The Effect of Magnesium Deficiency on Neurological Disorders: A Narrative Review Article.
Xue W1,2, You J2, Su Y2, Wang Q1,3.
Abstract
BACKGROUND:
Magnesium (Mg) is an essential element for the body. It is a cofactor for ATP, DNA, and RNA and more than 600 enzymes. As it is similar to Ca2+, this element can also act as a cell signaling molecule and play multiple important roles in the nervous, muscle, and immune systems. Recent studies have associated Mg-deficiency with many neurological disorders, such as cerebral vasospasm, Alzheimer’s disease, stroke, and migraine. As it plays such a crucial role in human body, therefore, we summarized the role of Mg in neurological disorders to illustrate the symptoms caused by Mg-deficiency and the possible underlying mechanisms.
METHODS:
We critically discuss the role of it that we review the recent literature of magnesium. We also review the available data which are concerning the role of magnesium in neurological disorders.
RESULTS:
Magnesium is related to neurological disorders on the basis of the study of animals and humans experiments. Furthermore, these nervous systems related diseases include cerebral vasospasm, Alzheimer’s disease, Parkinson’s disease, stroke and migraine.
CONCLUSION:
Magnesium has effects on neurological disorders, such as its utility in cerebral vasospasm, Alzheimer’s disease, Parkinson’s disease, stroke and migraine. So here we make a brief review to conclude it.
KEYWORDS:
Alzheimer’s disease; Magnesium; Migraine; Neurological disorders; Parkinson’s disease; Stroke PMID: 31223564 PMCID: PMC6570791
Magnesium in Prevention and Therapy.
Gröber U1, Schmidt J2, Kisters K3,4.
Abstract
Magnesium is the fourth most abundant mineral in the body. It has been recognized as a cofactor for more than 300 enzymatic reactions, where it is crucial for adenosine triphosphate (ATP) metabolism.
Magnesium is required for DNA and RNA synthesis, reproduction, and protein synthesis. Moreover, magnesium is essential for the regulation of muscular contraction, blood pressure, insulin metabolism, cardiac excitability, vasomotor tone, nerve transmission and neuromuscular conduction.
Imbalances in magnesium status-primarily hypomagnesemia as it is seen more common than hypermagnesemia-might result in unwanted neuromuscular, cardiac or nervous disorders.
Based on magnesium’s many functions within the human body, it plays an important role in prevention and treatment of many diseases. Low levels of magnesium have been associated with a number of chronic diseases, such as Alzheimer’s disease, insulin resistance and type-2 diabetes mellitus, hypertension, cardiovascular disease (e.g., stroke), migraine headaches, and attention deficit hyperactivity disorder (ADHD).
KEYWORDS:
ADHD; Alzheimer’s disease; asthma; cardiovascular disease; diabetes mellitus; hypomagnesemia; magnesium
The Role of Nutrients in Protecting Mitochondrial Function and Neurotransmitter Signaling: Implications for the Treatment of Depression, PTSD, and Suicidal Behaviors
Jing Du,1,3,*#Ming Zhu,1,*Hongkun Bao,1Bai Li,1Yilong Dong,1Chunjie Xiao,1Grace Y. Zhang,3Ioline Henter,4Matthew Rudorfer,2 and Benedetto Vitiello2
Abstract
Numerous studies have linked severe stress to the development of major depressive disorder (MDD), and suicidal behaviors.
Furthermore, recent preclinical studies from our laboratory and others have demonstrated that in rodents, chronic stress and the stress hormone cortisol has caused oxidative damage to mitochondrial function and membrane lipids in the brain.
Mitochondria play a key role in synaptic neurotransmitter signaling by providing adenosine triphosphate (ATP), mediating lipid and protein synthesis, buffering intracellular calcium, and regulating apoptotic and resilience pathways.
Membrane lipids are similarly essential to central nervous system (CNS) function, because cholesterol, polyunsaturated fatty acids, and sphingolipids form a lipid raft region, a special lipid region on the membrane that mediates neurotransmitter signaling through G-protein coupled receptors and ion channels.
Low serum cholesterol levels, low antioxidant capacity, and abnormal early morning cortisol levels are biomarkers consistently associated with both depression and suicidal behaviors.
In this review, we summarize the manner in which nutrients can protect against oxidative damage to mitochondria and lipids in the neuronal circuits associated with cognitive and affective behaviors.
These nutrients include ω3 fatty acids, antioxidants (vitamin C and zinc), members of the vitamin B family (Vitamin B12 and folic acid) and magnesium. Accumulating data have shown that these nutrients can enhance neurocognitive function, and may have therapeutic benefits for depression and suicidal behaviors. A growing body of studies suggests the intriguing possibility that regular consumption of these nutrients may help prevent the onset of mood disorders and suicidal behaviors in vulnerable individuals, or significantly augment the therapeutic effect of available antidepressants. These findings have important implications for the health of both military and civilian populations.
Keywords: vitamin, oxidative stress, synaptic plasticity, lipid, suicide, zinc
The Severity of Depressive Symptoms vs. Serum Mg and Zn Levels in Postmenopausal Women
M. Stanisławska, M. Szkup-Jabłońska, A. Jurczak, S. Wieder-Huszla, A. Samochowiec, A. Jasiewicz, I. Noceń, K. Augustyniuk, A. Brodowska, B. Karakiewicz, D. Chlubek, and E. Grochans
Abstract
The aim of this study was to assess the severity of depressive symptoms in postmenopausal women, depending on serum Mg and Zn levels.
The study involved 171 postmenopausal women from Poland, who were not using menopausal hormone therapy (MHT). The intensity of depressive symptoms was evaluated using a standard research technique, the Beck Depression Inventory (BDI).
The plasma Mg and Zn concentrations were measured. Depressive symptoms of different severity levels were diagnosed in 36.8 % of the women. The mean serum Mg level was 1.53 ± 0.28 mg/dL, and Zn level was 72 ±14 μg/dL.
The women with higher serum Mg and Zn levels had less depressive symptoms, and this observation is a precious information which can be used when planning depressive disorder prevention programmes.
Keywords: Depressive disorder, Postmenopause, Magnesium, Zinc
Magnesium in addiction – a general view.
Abstract
Addiction is a dysregulation of brain reward systems that progressively increases, resulting in compulsive drug use and loss of control over drug-taking.
Addiction is a brain disease.
There is evidence that magnesium deficit is involved in addiction to various addictive substances (heroin, morphine, cocaine, nicotine, alcohol, caffeine, and others). Magnesium is involved in all the stages of addiction. Magnesium deficit enhances the vulnerability to psychoactive substance addiction. Stress and trauma reduce the brain magnesium level and at the same time favor addiction development.
In experimental studies, administration of magnesium while inducing morphine dependence in rats reduced the dependence intensity. Magnesium reduces the NMDA receptor activity and the glutamatergic activity. Because stress and trauma induce hypomagnesemia with increased vulnerability to addiction, magnesium intake by people who are under prolonged stress could be a way to reduce this vulnerability and the development of addiction to different psychoactive substances.
Anxiety and depression appear to be associated with increases in drug-related harm and addictive substance use. Magnesium anxiolytic effect could be important for the antiaddictive action. Addiction is characterized by relapses. Magnesium deficiency may be a contributing factor to these relapses.
KEYWORDS:
addiction; cocaine; heroin; magnesium deficit; nicotine; stress; trauma
Efficacy of intravenous magnesium sulfate in the treatment of acute migraine attacks.
Demirkaya S1, Vural O, Dora B, Topçuoğlu MA.
Abstract
OBJECTIVE:
To study the efficacy and tolerability of 1 g of intravenous magnesium sulfate as acute treatment of moderate or severe migraine attacks.
BACKGROUND:
Migraine is a common disorder in which not only the pain but also the accompanying symptoms such as nausea and vomiting reduce activity and productivity of sufferers. Many drugs used for the treatment of acute migraine attacks have many side effects, are not well tolerated, are ineffective in some patients, or cannot be used during pregnancy or in patients with ischemic heart disease. Magnesium deficiency has been proposed to play a role in the pathophysiology of migraine, and recently treatment of migraine with magnesium has gained considerable interest.
METHODS:
This was a randomized, single-blind, placebo-controlled trial including 30 patients with moderate or severe migraine attacks. Fifteen patients received 1 g intravenous magnesium sulfate given over 15 minutes. The next 15 patients received 10 mL of 0.9% saline intravenously. Those in the placebo group with persisting complaints of pain or nausea and vomiting after 30 minutes also received 1 g magnesium sulfate intravenously over 15 minutes. The patients were assessed immediately after treatment, and then 30 minutes and 2 hours later. Intensity of pain, accompanying symptoms, and side effects were noted.
RESULTS:
All patients in the treatment group responded to treatment with magnesium sulfate. The pain disappeared in 13 patients (86.6%); it was diminished in 2 patients (13.4%); and in all 15 patients (100%), accompanying symptoms disappeared. In the placebo group, a decrease in pain severity but persisting nausea, irritability, and photophobia were noted in 1 patient (6.6%). Accompanying symptoms disappeared in 3 patients (20%) 30 minutes after placebo administration. All patients initially receiving placebo were subsequently given magnesium sulfate. All of these patients responded to magnesium sulfate. In 14 patients (93.3%), the attack ended; in 1 patient (6.6%), pain intensity decreased; and in all 15 patients (100%), accompanying symptoms disappeared. Both the response rate (100% for magnesium sulfate and 7% for placebo) and the pain-free rate (87% for magnesium sulfate and 0% for placebo) showed that magnesium sulfate was superior to placebo. Twenty-six patients (86.6%) had mild side effects which did not necessitate discontinuing treatment during magnesium sulfate administration.
CONCLUSION:
Our results show that 1 g intravenous magnesium sulfate is an efficient, safe, and well-tolerated drug in the treatment of migraine attacks. It is possible that magnesium sulfate could be used in a broader spectrum of patients than other drugs commonly used for attack treatment. In view of these results, the effect of magnesium sulfate in acute migraine should be examined in large-scale studies.
The Association between Serum Magnesium Levels and Depression in an Adult Primary Care Population
Emily K. Tarleton,1,*Amanda G. Kennedy,2Gail L. Rose,3Abigail Crocker,4 and Benjamin Littenberg5
Abstract
Depression is common, places a large burden on the patient, their family and community, and is often difficult to treat.
Magnesium supplementation is associated with improved depressive symptoms, but because the mechanism is unknown, it is unclear whether serum magnesium levels act as a biological predictor of the treatment outcome.
Therefore, we sought to describe the relationship between serum magnesium and the Patient Health Questionnaire (PHQ, a measure of depression) scores. A cross-sectional analysis of medical records from 3604 adults (mean age 62 years; 42% men) seen in primary care clinics between 2015 and 2018, with at least one completed PHQ were included.
The relationship between serum magnesium and depression using univariate analyses showed a significant effect when measured by the PHQ-2 (−0.19 points/mg/dL; 95% CI −0.31, −0.07; P = 0.001) and the PHQ-9 (−0.93 points/mg/dL; 95% CI −1.81, −0.06; P = 0.037).
This relationship was strengthened after adjusting for covariates (age, gender, race, time between serum magnesium and PHQ tests, and presence of diabetes and chronic kidney disease) (PHQ-2: −0.25 points/mg/dL; 95% CI −3.33, −0.09; P < 0.001 and PHQ-9: −1.09 95% CI −1.96 −0.21; P = 0.015).
For adults seen in primary care, lower serum magnesium levels are associated with depressive symptoms, supporting the use of supplemental magnesium as therapy. Serum magnesium may help identify the biological mechanism of depressive symptoms and identify patients likely to respond to magnesium supplementation.
Keywords: magnesium, depression, primary care
Correlation of magnesium intake with metabolic parameters, depression and physical activity in elderly type 2 diabetes patients: a cross-sectional study
Abstract
Background
Type 2 diabetes mellitus is a major global public health problem in the worldwide and is increasing in aging populations. Magnesium intake may be one of the most important factors for diabetes prevention and management. Low magnesium intake may exacerbate metabolic abnormalities. In this study, the relationships of magnesium intake with metabolic parameters, depression and physical activity in elderly patients with type 2 diabetes were investigated.
Methods
This cross-sectional study involved 210 type 2 diabetes patients aged 65 years and above. Participants were interviewed to obtain information on lifestyle and 24-hour dietary recall. Assessment of depression was based on DSM-IV criteria. Clinical variables measured included anthropometric measurements, blood pressure, and biochemical determinations of blood and urine samples. Linear regression was applied to determine the relationships of magnesium intake with nutritional variables and metabolic parameters.
Results
Among all patients, 88.6% had magnesium intake which was less than the dietary reference intake, and 37.1% had hypomagnesaemia. Metabolic syndromes and depression were associated with lower magnesium intake (p < 0.05). A positive relationship was found between magnesium intake and HDL-cholesterol (p = 0.005). Magnesium intake was inversely correlated with triglyceride, waist circumference, body fat percent and body mass index (p < 0.005). After controlling confounding factor, HDL-cholesterol was significantly higher with increasing quartile of magnesium intake (p for trend = 0005). Waist circumference, body fat percentage, and body mass index were significantly lower with increase quartile of magnesium intake (p for trend < 0.001). The odds of depression, central obesity, high body fat percentage, and high body mass index were significantly lower with increasing quartile of magnesium intake (p for trend < 0.05). In addition, magnesium intake was related to high physical activity level and demonstrated lower serum magnesium levels. Serum magnesium was not significantly associated with metabolic parameters.
Conclusions
The majority of elderly type 2 diabetes who have low magnesium intake may compound this deficiency with metabolic abnormalities and depression. Future studies should determine the effects of increased magnesium intake or magnesium supplementation on metabolic control and depression in elderly people with type 2 diabetes.
Keywords: Magnesium, Diabetes, Metabolic control, Depression, Physical activity, Elderly
Magnesium for treatment-resistant depression: a review and hypothesis. – PubMed
Abstract
Sixty percent of cases of clinical depression are considered to be treatment-resistant depression (TRD). Magnesium-deficiency causes N-methyl-d-aspartate (NMDA) coupled calcium channels to be biased towards opening, causing neuronal injury and neurological dysfunction, which may appear to humans as major depression.
Oral administration of magnesium to animals led to anti-depressant-like effects that were comparable to those of strong anti-depressant drugs. Cerebral spinal fluid (CSF) magnesium has been found low in treatment-resistant suicidal depression and in patients that have attempted suicide. Brain magnesium has been found low in TRD using phosphorous nuclear magnetic resonance spectroscopy, an accurate means for measuring brain magnesium. Blood and CSF magnesium do not appear well correlated with major depression.
Although the first report of magnesium treatment for agitated depression was published in 1921 showing success in 220 out of 250 cases, and there are modern case reports showing rapid terminating of TRD, only a few modern clinical trials were found.
A 2008 randomized clinical trial showed that magnesium was as effective as the tricyclic anti-depressant imipramine in treating depression in diabetics and without any of the side effects of imipramine. Intravenous and oral magnesium in specific protocols have been reported to rapidly terminate TRD safely and without side effects.
Magnesium has been largely removed from processed foods, potentially harming the brain.
Calcium, glutamate and aspartate are common food additives that may worsen affective disorders.
We hypothesize that – when taken together – there is more than sufficient evidence to implicate inadequate dietary magnesium as the main cause of TRD, and that physicians should prescribe magnesium for TRD.
Since inadequate brain magnesium appears to reduce serotonin levels, and since anti-depressants have been shown to have the action of raising brain magnesium, we further hypothesize that magnesium treatment will be found beneficial for nearly all depressives, not only TRD.
https://www.ncbi.nlm.nih.gov/pubmed/19944540
ChooseLife : Has there ever been a more important time to eat your greens? Make Green Smoothies? Take Epsom Salts baths? or, a few grains of Epsom Salts in drinking water through the day?

4 Replies to “Magnesium – Mental Health Research Reviews”